Positional Vertigo: Could It Be Migraine Related?
The authors present a brief background on migraines as well as a case history of a possible vestibular migraine
A migraine is a common and disabling neurologic disorder.1 When we think about migraines, we typically think of strong and painful headache episodes. However, migraines can carry with them symptoms that are much broader than just headaches, and can be quite debilitating. As per the International Headache Society, migraines can be divided in two major sub-types: (1) migraine without aura and (2) migraine with aura. A typical aura consists of visual and/or sensory symptoms (for example, numbness) with and without speech symptoms. The complete reversibility of the symptoms characterizes the aura. Table 1 outlines the symptoms of both migraine sub-types.2 Migraines without aura are the most common. These are described as intense headache attacks lasting between 4 and 72 hours, and are characterized as unilateral (occurring on one side of the head), pulsatile in quality, painful, and generally exacerbated by physical activity. These types of migraines are also typically accompanied by sensitivity to light and sounds, as well as nausea. By contrast, migraines with aura are often described as a classical migraine accompanied by the gradual manifestation of one or a mix of visual, sensory and/or speech impairments. These symptoms typically last less than 60 minutes, and are all completely reversible.2
Table 1. Diagnostic criteria for migraines without aura and with aura
| Migraine without Aura | Migraine with Aura |
|---|---|
|
|
In some cases, migraines can cause vestibular symptoms, such as vertigo. The link between migraine and vertigo is well recognized in the literature.3–7 These types of migraines are known as vestibular migraines. Approximately 1% of the general population, 10% of patients seen in vestibular clinics and 9% of patients seen in migraine clinics are affected by such vestibular migraines.4 Recently, the committee for Classification of Vestibular Disorders of the Barany Society and the Migraine Classification Subcommittee of the International Headache Society (IHS) jointly formulated a list of diagnostic criteria for vestibular migraines.5 These are outlined in Table 2. In a recent study of 147 patients with varied vestibular diagnoses, including Ménière’s disease (MD), vestibular migraines (VM), Ménière’s disease plus vestibular migraine (MDVM) and chronic subjective dizziness, 48% (71 patients) were diagnosed with a vestibular migraine alone. In these patients 38% complained of hearing problems (i.e., subjective hearing loss, aural pressure, tinnitus). No temporal relationship between symptoms of vertigo/dizziness and headaches were found. In other words, this means that the headaches could occur before, during, after, or between the vestibular episodes.6
Table 2. Diagnostic criteria for vestibular migraines
Note: that the vestibular migraine criteria include the following symptoms: spontaneous vertigo, positional vertigo, visually induced vertigo, head motion-induced vertigo and head motion-induced dizziness. |
Since vestibular migraines include positional vertigo (occurring after a change of position) it can be hard to differentiate a diagnosis of vestibular migraine from benign paroxysmal positional vertigo (BPPV). BPPV is the most common cause of vertigo.8 BPPV is a vestibular disorder of the inner ear which is characterized by repeated episodes of positional vertigo.9 In BPPV, the otoconia of the inner ear become dislodged from the macula and migrate to the semi-circular canals. When the person moves his/her head in the plane of the affected semi-circular canal, the free-floating otoconia causes a more intense movement of the endolymphatic fluid in that specific canal, thereby inducing brief rotational vertigo and spells of nausea.10 Diagnosis of BPPV is usually obtained by performing a positional test, such as the Dix-Hallpike test.11 The Dix-Hallpike is a maneuver where the patient is asked to sit upright on a bed with legs extended. In order to perform the Dix-Hallpike to assess the right posterior canal, the examiner positions the head of the patient at a 45° angle to the right and lays the patient down on his/her back. In this way, the nose is facing up and the undermost ear is the right ear (for pictures and details see Jacobson and Shepard12). If a right BPPV is present, then given the physiology of the vestibular-ocular pathway, the dislodged otoconias that are floating in the right posterior canal should induce a brief torsional geotropic nystagmus (beating toward the ground). See Figure 1 for an illustration of the direction of the nystagmus. The nystagmus occurs because the Dix-Hallpike maneuver displaces the otoconia toward one direction. The symptoms disappear when the otoconias stop moving in the canal.
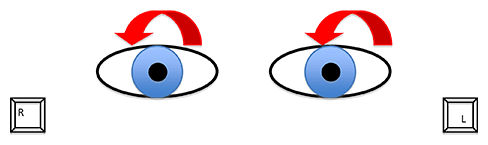
Figure1. Direction of the nystagmus observed when patient is tested positive for a right posterior canal BPPV with the Dix-Hallpike maneuver. We observe a torsional nystagmus (up and right beating nystagmus).
BPPV is successfully treated with a particle repositioning maneuvers, called the Epley maneuver.12 This maneuver aims to reposition the otoconia to their original state, by forcing them to move or float from one semi-circular canal, back into the utricle from where they were dislodged.
Migrainous vertigo symptomatology is often very similar (even identical) to positional vertigo and thus, raises the probability of a misdiagnosis. Studies have shown that BPPV is highly associated with migraines, and that individuals suffering from migraines are three times more likely to develop BPPV than their counterparts who are not affected by migraines.13 Despite the similarities of both pathologies, the literature has provided two key aspects to differentially diagnosed BPPV from vestibular migraines8,13: (1) the direction of the nystagmus and (2) the duration of the symptoms. The BPPV is revealed by a geotropic nystagmus with short duration. As previously explained, as soon as the otoconia stop moving during positional testing, the nystagmus should disappear. In the case of migrainous vertigo or vestibular migraines, the direction of the nystagmus is usually atypical during positional testing (nystagmus in a direction that is not associated with any semi-circular canal) and lasts as long as the patient stays in the same position. As mentioned previously, BPPV can be treated with repositioning maneuver but this type of treatment as no effect on vestibular migraines. Practitioners need to be cautious with their diagnostic of BPPV. Even though the maneuver in itself won’t harm the patient if performed properly, a misdiagnosis with vestibular migraine will result in weeks of repositioning maneuver with no improvement of the symptoms and unreasonable delay of referral to a neurologist.
Clinical Case
In this section, we will present a clinical case study. This patient was seen for complaints of dizziness and hearing fluctuation and presented an interesting case because it outlined the difficulties we encounter when evaluating a patient with a possible vestibular migraine.
Case History
The patient was a 58-year-old woman who was referred by her ENT for recent complaints of intermittent dizziness. She reported that, in the last month, she had an intermittent sensation of fullness in her left ear that lasted a few hours. This aural fullness seemed to be accompanied by a feeling of “lightheadedness.” During these episodes, she reported that fast movements of her head exacerbated the sensation of dizziness. She reported intermittent occurrence of the symptoms with good days, where she didn’t experienced any oral fullness and/or light-headedness, and bad days, when both symptoms were present. A dynamic visual environment (visual moving scene) was not reported as a trigger of the symptoms.
Her symptoms would last about a day and usually started in the morning with a sensation of aural fullness in her left ear and high-pitched tinnitus in that ear. The fullness sensation gradually subsided during the afternoon. In the evening, she reported frontal headaches for which she had to stop all activities and rest. She reported having about three headaches per week. On her “bad days” she indicated sensitivity to both, high pitch sounds and light. She was in good general health and did not take medication on a regular basis.
Results
The patients hearing thresholds are outlined in Figure 2.
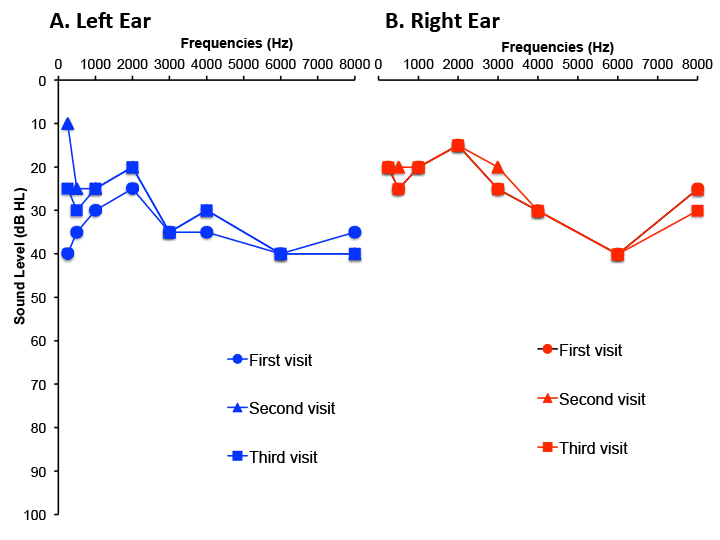
Figure 2. Hearing thresholds obtained at three visits for the left (A) and right (B) ears. Variations of threshold at 250 Hz and 500 Hz were observable between each testing session only in the left ear (A).
On the day of the first evaluation, the patient was having a “bad day.” The hearing evaluation revealed a normal tympanogram in the left ear and negative pressure with normal compliance in the right ear. Acoustic reflex thresholds were within normal range for the left ipsilateral and right contralateral conditions, but could not be tested in the right ear because a seal could not be maintained with the probe in that ear. Audiometric thresholds, shown by the round symbols in Figures 2A and B revealed a mild flat sensorineural hearing loss in the left ear and a mild mostly conductive hearing loss at 500Hz and in high frequencies ranging from 3kHz to 8kHz in the right ear.
The Dix-Hallpike maneuver was then performed to allow us to assess the function of the posterior canals for BPPV. That test was positive on the right side only, but the nystagmus was not torsional, it was ageotropic (beating away from the ground). As previously indicated, non-torsional ageotropic nystagmus is not typically associated with BPPV. Still, we decided to perform an Epley maneuver (particle-repositioning maneuver) and re-evaluate the condition of the patient a few days later. If the pathology of the patient was a true BPPV, then the repositioning maneuver should have reversed and treated the symptoms.
A few days later, the patient came back for a follow-up visit. At that time, the patient stated that she was having a “good day.” Tympanometric results were similar to the last test in both ears. An audiogram was performed, and low frequency thresholds (250 Hz and 500 Hz) in the left ear were significantly improved. Positional testing was then performed, and this time, the Dix-Hallpike maneuver was negative for the right side, but positive for the left side. The nystagmus was now non-fatigable (i.e., lasted as long as the patient stayed in the same position) and ageotropic. We did not perform any particle repositioning maneuver, and decided to follow up again a few days later.
On the day of the third evaluation, the patient was having a “bad day,” but described her symptoms as being “not as bad as the first evaluation.” We performed another audiogram and this time, we noted a mild but not significant decrease in the low frequencies on the left side, compared to the last audiogram. These thresholds were still better than what they were on the day of the first assessment. The thresholds of the right ear remained unchanged. We performed the positional testing, and this time, the patient showed a non-fatigable ageotropic nystagmus on both the right and left sides.
Given the variability in the test results with all assessments, and the history of migraines and dizziness, we decided to refer this patient for a migraine assessment with a neurologist. We have yet to hear back about the outcomes of this case study from the neurologists, but we keep in mind that our patient reported debilitating symptoms of migraines (headaches, light and sound sensitivity during bad days), which we believe cannot be ignored and warrant further investigation. Moreover, positional testing revealed symptoms of nystagmus which did not correlate with a peripheral pathology. We believe that misinterpretation of the positional testing may result in errors in the identification of the origin of the vertigo symptoms and ultimately to mismanagement of the patient’s symptoms.
Conclusion
In the present article, we present a brief background on migraines as well as a case history of a patient with a possible vestibular migraine (still to be confirmed by neurologist) to indicate the complexity of differentially diagnosing peripheral vestibular impairments. We hope that this article serves to raise awareness of the link that exists between vertigo/dizziness and migraines in order to help clinicians better understand these impairments, and in turn offer the best care to patients who suffer from such conditions.
As audiologists we will meet patients with similar complains of dizziness associated with headaches. We have to be aware of conditions such as vestibular migraines, so that we can make appropriate decisions about which diagnostic tests to perform and which intervention strategies to employ. Audiologists need to be able to investigate whether the symptoms of dizziness or vertigo are due to pathologies in the peripheral vestibular system (Ménière’s disease or positional vertigo) or the central nervous system. This task can sometimes be difficult since different types of pathologies (vestibular migraine, BPPV, Ménières disease, etc.) share common symptoms and mimic one another. In those particular cases, misdiagnosis by clinicians is not uncommon. As audiologists, we have a responsibility to fully and carefully investigate all of the different symptoms presented by a patient in order to make the right clinical decisions, and follow the right course of treatment or referral.
References
- Olesen J, Steiner TJ The International Classification Of Headache Disorders 2nd Edition. Oxford: International Headache Society; 2004.
- The International Classification of headache disorders, 3rd edition (beta version). Cephalalgia 2013;33:629–808.
- Cha YH, Lee H, Santell LS, Baloh RW. Association of benign recurrent vertigo and migraine in 208 patients. Cephalalgia 2009;29:550–5.
- Lempert T, Neuhauser H. Epidemiology of vertigo, migraine and vestibular migraine. J Neurol 2009;256:333–8.
- Lempert T, Olesen J, Furman J, Waterson J, Seemungal B, et al. Vestibular migraine: Diagnostic criteria. J Vestib Res 2012;22:167–72.
- Neff BA, Staab JP, Eggers SD, Carlson ML, Schmitt WR, et al. Auditory and vestibular symptoms and chronic subjective dizziness in patients with Ménière's disease, vestibular migraine, and ménière's disease with concomitant vestibular migraine. Otol Neurotol 2012;33:1235–44.
- Neuhauser H, Lempert T. Vestibular Migraine. Neurologic clinics 2009;27:379–91.
- von Brevern M, Radtke A, Clarke AH, Lempert T. Migrainous vertigo presenting as episodic postiional vertigo. Neurology 2004;62:469–72.
- Bhattacharyya N, Baugh R, Orvidas L, Barrs D, Bronston L, et al. Clinical practice guideline: Benign paroxysmal positional vertigo. Otolaryngol Head Neck Surg 2008;139:S47–81.
- Cha YH, Baloh RW. Migraine Associated Vertigo. Journal of clinical neurology 2007;3:121–26.
- Hunt W, Zimmermann E, Hilton M. Modifications of the Epley (canalith repositioning) manoeuvre for posterior canal benign paroxysmal positional vertigo (BPPV). Cochrane Database Syst Rev 2012:1–43.
- Jacobson GP, Shepard NT. Balance function assessment and management; Stach B, editor. San Diego: Plural Publisher; 2008.
- Roberts RA, Gans RE, Kastner AH. Differentiation of migrainous positional vertigo (MPV) from horizontal canal benign paroxysmal positional vertigo (HC-BPPV). Int J Audiol 2006;45: 224–26.


