Signia Active: The Beginning of An Era of Hearing Without Stigma
Andre Marcoux1, Michele Dostaler1 and Daniel Olesen2
1 WS Audiology Canada Inc., Burlington, Canada
2 WS Audiology Inc., Lynge, Denmark
The acoustic amplification of sounds by hearing aids is the most common corrective strategy for the management of hearing loss, with satisfaction rates among users surpassing 80% (Powers & Rogin, 2019). Despite their efficacy, only one third of candidates for hearing aids will purchase and use them (Bainbridge & Ramachandran, 2014; Powers & Rogin 2019). Various reasons for postponing or rejecting the use of hearing aids include their cost, their perceived lack of benefit, denial of sufficient hearing loss to warrant their ongoing use and, finally, the negative stigma associated with hearing loss and hearing aids (Powers & Rogin, 2019). While significant technological strides have been made by hearing aid manufacturers to provide affordable and versatile solutions which deliver a more natural sound in a variety of listening situations, these efforts have only provided a modest improvement with respect to overall end user adoption. This observation may be partly explained by the remaining unresolved issues around the aesthetics of hearing aids and their stigmatization potential. In fact, of all objections related to hearing aid use, the most difficult to counteract with facts and evidence may be those provided by a candidate with perceived stigma (Johnson et al., 2005; Wallhagen, 2009).
As offered by Crocker et al. (1998), stigma can be defined as the possession of, or belief that one possesses, an attribute or characteristic that conveys a social identity that is devalued in a particular social context. In the case of hearing impairment, stigma is formed around the implication of disability and ageism (Barnett et al, 2017). By extension, this can also implicate additional problems that strengthen the stigma, such as lower academic achievement, limitations in social engagement, poor self-esteem, and emotional difficulties (Privado, Carasco & Duran, 2019). While the stigmatized person may not be able to verify that others share the same stigmatizing beliefs, they feel threatened by the potential discrimination, labels, and negative stereotypes of their condition in a social context (Major & O’Brien, 2005). Such justifications are difficult to argue when too often stigma is exacerbated by the entertainment industry which depict hearing loss as comical, embarrassing, lonely, and threatening to one’s work (Foss, 2014).
Despite efforts at the societal and professional levels to reduce stigma by dispelling some of its erroneous constructs, stigma remains a significant barrier towards the adoption of hearing aids (Barnett et al, 2016). Individuals with hearing loss who feel stigmatized by their condition may refuse to wear hearing aids for fear of compromising their social identify and, in some cases, may adopt stigmatic behaviors such as avoiding challenging communication settings altogether (Hallberg & Barrenas, 1995; Hallberg & Jansson, 1996). Such stigmatic behaviors have been found to contribute to conditions of loneliness (Shukla et al., 2020; Weinstein, Sirow & Moser, 2016), depression (Boi et al., 2012), reduced quality of life (Ciorba et al., 2012) and cognitive decline (Amieva et al., 2015; Dawes et al., 2015; Lin et al., 2013). Those who, despite stigma, accept the use of hearing aids to minimize such negative consequences will often request that they be concealed (David, Zoizner & Werner, 2018).
While concealment is often viewed as the only means to negate the identification of a hearing aid, several other strategies are applied during the design of hearings aids to reduce or negate their stigmatization potential and consequently to increase their adoption from individuals with stigma. These consist of device interaction, de-identification, and normalization.
Device concealment
This design strategy has been developed and refined since the introduction of the modern electronic hearing aid insofar as it relates to the ongoing miniaturization of the hearing aid and the physical area it occupies on the ear of the user. Other examples of concealment include disguising the device with colours that blend with skin tones, or the introduction of the Receiver-In-the-Canal (RIC) which eliminated the need for larger, more visible sound tubes and permitted the miniaturization of the hearing aid housing by relocating the receiver into the ear canal. While concealment has been an effective design strategy in reducing the stigmatizing potential of hearing aids, the resulting miniaturization also presents its challenges and trade-offs. Smaller devices may not allow for larger batteries or receivers to provide the necessary power to correct more severe levels of hearing loss. Also, smaller devices may not have sufficient space to accommodate all the necessary sensors, circuits, and antennas to provide the same level of functionality the consumer has come to expect from slightly larger devices. For example, an invisible device which fits deeply into the ear canal may not have a sufficiently large footprint to accommodate an antenna for Bluetooth communication nor have sufficient line-of-sight for adequate reception and transmission.
Device interaction
By permitting the interaction between the hearing aid with peripheral non-stigmatizing devices, the stigmatization potential of the hearing aid can be reduced. Early examples of device interaction include the wireless connectivity with remote controls, television transmitters and remote microphones. More recently, hearing aids can be paired with the user’s smartphone which are associated with attributes of being youthful and “techy”. In so doing, music and telephone calls can be directly streamed to the hearing aid, or using dedicated apps, can permit to control hearing aid settings and even connect directly with hearing healthcare professionals for on-demand virtual adjustments.
Device de-identification
The purpose of device de-identification is to remove and modify the most identifiable features from the device as a means of decreasing its visibility and confusing any observer. The Signia Styletto is a perfect example of device de-identification. By removing the volume wheels and switches, as well as redesigning the housing of the hearing aid from the traditional oblong shape to one which is streamlined and elongated, the Styletto does not have the appearance of a typical behind-the-ear hearing aid.
Device normalization
The process of normalization is to redesign the stigmatizing device to become indistinguishable from a non-stigmatizing target device. In 2015, the world’s first wireless earbuds were introduced to the market. These were quickly adopted by electronic and music aficionados alike to stream sound from their smartphones without the hassle of wires or large over-the-ear headphones. While earbuds were not designed to address hearing loss per se, a normalization vector was nonetheless created. Following this vector, hearing aids can be made indistinguishable from wireless earbuds and thus be worn and operated by those with stigma in a manner that they would perceive to be better aligned with their pre-conceived societal norms of an observer.
A world’s first in the normalization of the full-prescription hearing aid
Signia was first to introduce the concept of device normalization to the market with the release of Signia Active; the world’s first full-prescription earbud. Signia Active represents a milestone for the industry by which stigma can be greatly reduced for those requiring hearing aids, thereby increasing the adoption rate of hearing aids which has historically been stunted by such objections. Also, because Signia Active does not need to be concealed deep inside the ear canal to reduce stigma, it allows significantly more functionality to improve overall consumer satisfaction, including full connectivity, rechargeability and dual microphones.
To substantiate the claim that Signia Active does indeed reduce stigma for individuals living with hearing loss, a study was performed to determine their perceptions towards hearing aids, including the Signia Active. A sample of 384 Canadian respondents were recruited to complete an online questionnaire. Respondents were required to report hearing loss, as defined by the self-stated hearing loss questionnaire by Kochkin and Bentler (2010), hearing aid ownership, hearing loss diagnosis, previous interaction with hearing care dispensers, as well as their gender and age. Otherwise, no respondents were excluded once the totality of criteria were met. Furthermore, none of the respondents were affiliated with the hearing aid industry or had any direct contact with or knowledge of Signia and its parent company during the questionnaire completion process. The median completion time was 11.7 minutes.
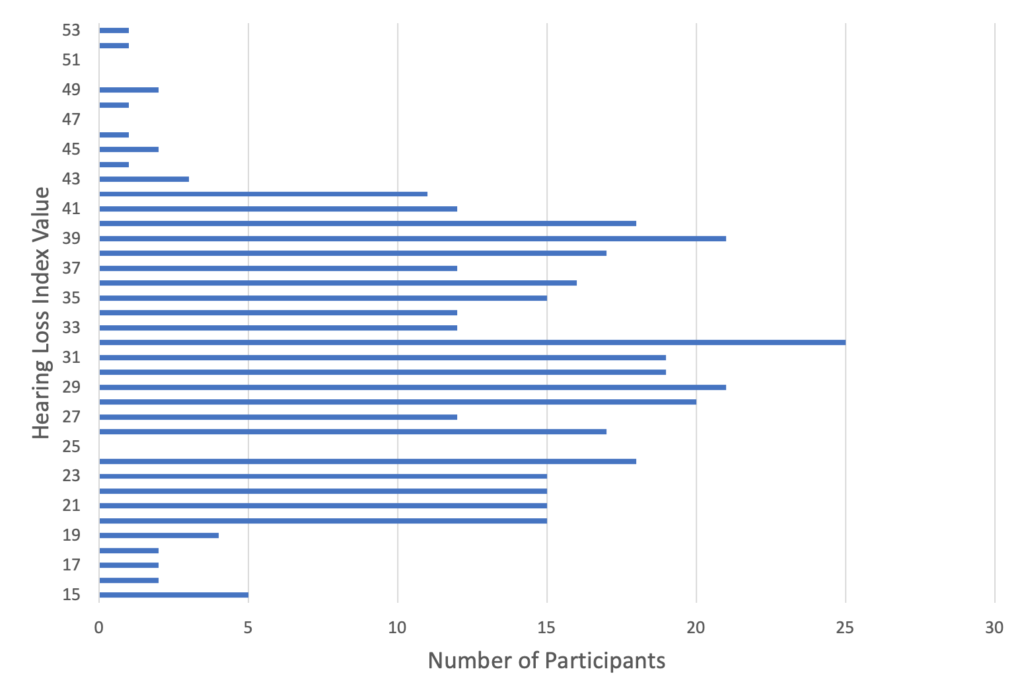
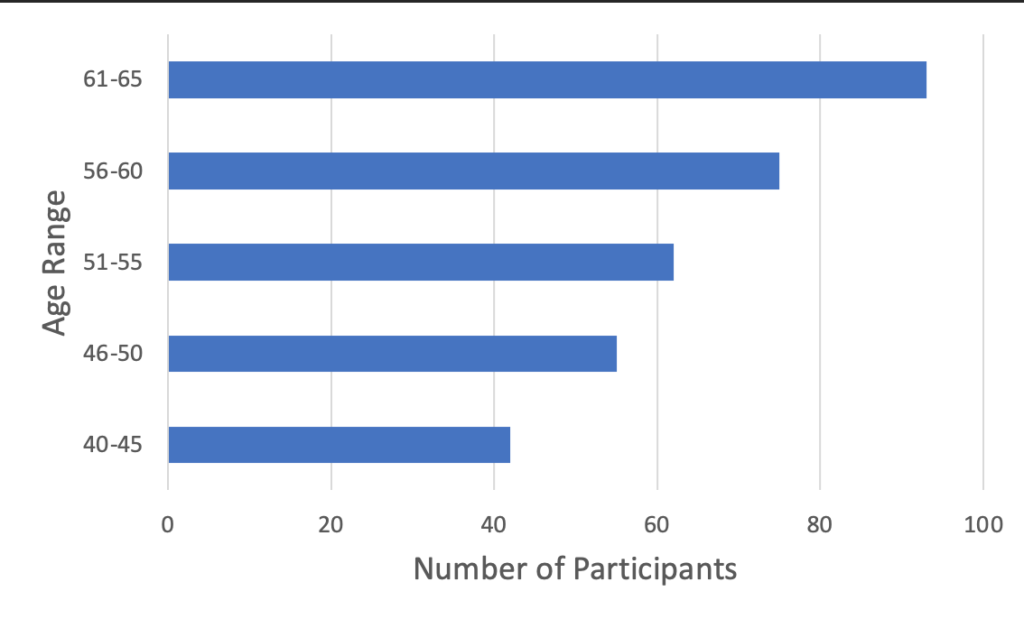
Figure 1 shows results from the self-reported hearing loss questionnaire (Kochkin & Bentler, 2010) covering a range of values from 15 to 53, with a median value of 31, indicative of individuals with mild to moderate hearing loss. Close to 30% of participants were hearing aid owners with 25% having owned them for more than 3 months and 5% having owned them for 3 months or less. Approximately 7% of participants were currently in a hearing aid trial period, while 64% had never owned a hearing aid. The median age of participants was 59 years, with a distribution which skews slightly towards the older ages, as shown in Figure 2. The gender split was 60% male and 40% female.
A diagnosis of hearing loss was provided by a professional in 63% of cases, of which 37% were identified as an audiologist or doctor in a hearing clinic, 9% as a hearing aid professional in a retail setting, 8% by an ENT, 7% by a general practitioner, and 2% by another type of professional.
The results from the questionnaire are separated in two publications. The current publication, reports findings from one of the questions from the overall questionnaire. Results from the other sections of the questionnaire are reported in a future publication. Participants were presented with pictures of 8 ear-worn devices and provided with the following statement: “Below you see 8 products. Please select the devices that you think are hearing aids by clicking on their picture.” For each device, a stand-alone picture, as shown in Figure 3a, as well as both side and rear views of the device worn by the same male individual, as shown in Figure 3b, were provided. As listed in Figure 3a, six of the eight devices were Signia hearing aids, while the other devices were the commercially available earbuds Apple Airpods and Bose Sport Earbuds.

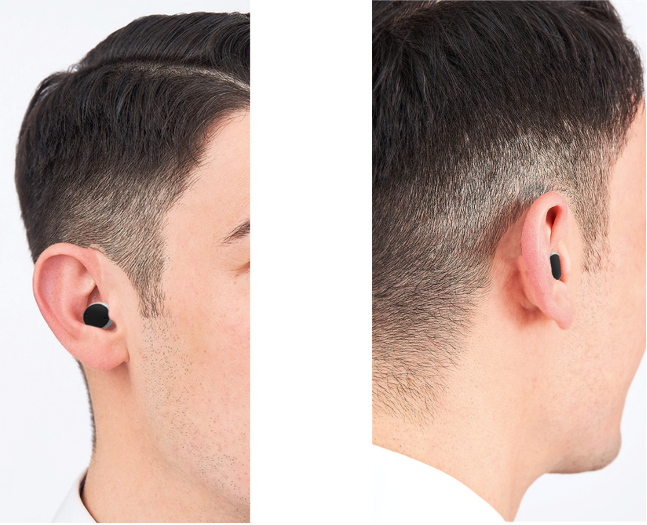
Figure 4 provides participants’ association frequencies for each device. Results indicate that the behind-the-ear devices are those most associated as being hearing aids. The in-the-ear hearing aids, both the Signia Insio ITC and Signia Silk were identified as hearing aids in approximately half of cases. It should be noted that Signia Silk is the smallest of all the hearing aids within this group and can be concealed within an ear canal. Despite its small size, its association as a hearing aid remains for more than half of the study participants. Those with the lowest association with hearing aids were the two commercially available earbuds as well as the Signia Active.
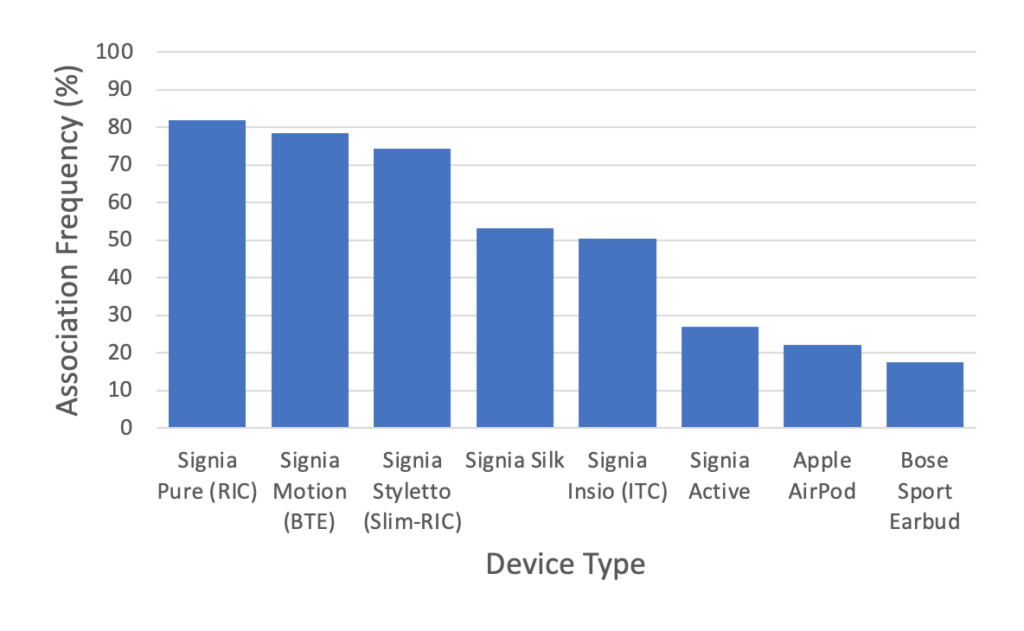
Interestingly, the Signia Active was associated to a hearing aid with a similar frequency as the Apple Airpods, which is not a hearing aid whatsoever. Further analyses using the Related-Samples McNemar Change Test confirm that that the association frequencies of Signia Active and Apple AirPods at 26.8% and 22.1% respectively are not significantly different (X2(1)=2.491, p>.05). This result indicated that the Signia Active and Apple Airpod are identified as hearing aids to the same extent. This result applies to participants who are both users and non-users of hearing aids (X2(1)=0.074, p>.05).
These results clearly demonstrate that Signia Active is identified as a hearing aid the least often amongst all form factors, including those which can be concealed. Furthermore, Signia Active is identified as a hearing aid to the same extent as a listening device that is not intended for individuals with hearing loss. In conclusion, our results suggest that Signia Active does not possess the same degree of stigmatizing potential attributable to other hearing aids.
While stigmatized individuals with hearing loss may still prefer to conceal their hearing aid, Signia Active provides a suitable alternative which does not compromise on functionality as do smaller concealable devices. Signia Active provides a level of sound processing and connectivity which is unattainable with smaller devices which cannot accommodate or provide proper positioning of the required components.
Consumers themselves, whether stigmatized by hearing loss or not, will recognize that Signia Active appears to resemble earbuds worn by the general population and consequently infer that they will not be identified as hearing aids by any observer. Results from the current study can also be used by hearing care professionals to stimulate a conversation with the consumer when stigma is suspected or relayed. While the authors agree that proper counselling should be provided to consumers to address stigma, Signia provides world leading innovation for those who would otherwise delay or reject amplification and strives to ensure that all individuals with hearing loss can fully enjoy and participate in life without barriers.
References
- Amieva, H., Ouvrard, C., Giulioli, C., Meillon, C., Rullier, L., & Dartigues, J. F. (2015). Self-reported hearing loss, hearing aids, and cognitive decline in elderly adults: A 25-year study. Journal of the American Geriatrics Society, 63(10), 2099–2104.
- Bainbridge, K. E., & Ramachandran, V. (2014). Hearing aid use among older U.S. adults; the national health and nutrition examination survey, 2005-2006 and 2009-2010. Ear and Hearing, 35(3), 289–294.
- Barnett, M., Hixon, B., Okwiri, N., Irungu, C., Ayugi, J., Thompson, R., Shinn, J. B., & Bush, M. L. (2017). Factors involved in access and utilization of adult hearing healthcare: A systematic review. Laryngoscope, 127(5), 1187-1194
- Boi, R., Racca, L., Cavallero, A., Carpaneto, V., Racca, M., Dall' Acqua, F., Ricchetti, M., Santelli, A., & Odetti, P. (2012). Hearing loss and depressive symptoms in elderly patients. Geriatrics & Gerontology International, 12(3), 440–445.
- Ciorba, A., Bianchini, C., Pelucchi, S., & Pastore, A. (2012). The impact of hearing loss on the quality of life of elderly adults. Clinical Interventions in Aging, 7, 159–163.
- Crocker, J., Major, B. and Steele, C. (1998) Social Stigma. In: Gilbert, D. T., Fiske, S. T. & Lindzey, G., Eds., The Handbook of Social Psychology, 4th Edition, Vol. 2. Academic Press, New York, 504-553.
- David, D., Zoizner, G., & Werner, P. (2018). Self-Stigma and age-related hearing loss: A qualitative study of stigma formation and dimensions. American Journal of Audiology, 27(1), 126–136.
- Dawes, P., Emsley, R., Cruickshanks, K. J., Moore, D. R., Fortnum, H., Edmondson-Jones, M., McCormack, A., & Munro, K. J. (2015). Hearing loss and cognition: The role of hearing aids, social isolation and depression. PloS one, 10(3), e0119616.
- Foss, K. A. (2014) (De)stigmatizing the silent epidemic: Representations of hearing loss in entertainment television, Health Communication, 29(9), 888-900.
- Hallberg, L. R., & Barrenas, M. L. (1995). Coping with noise-induced hearing loss: Experiences from the perspective of middle-aged male victims. British Journal of Audiology, 29(4), 219-230.
- Hallberg, L. R., & Jansson, G. (1996). Women with noise-induced hearing-loss: An invisible group? British Journal of Audiology, 30(5), 340-345.
- Johnson, C. E., Danhauer, J. L., Gavin, R. B., Karns, S. R., Reith, A. C., & Lopez, I. P. (2005). The "hearing aid effect" 2005: A rigorous test of the visibility of new hearing aid styles. American Journal of Audiology, 14(2), 169-175.
- Kochkin, S., & Bentler, R. (2010). The validity and reliability of the BHI Quick Hearing Check. Hearing Review, 17(12), 12-28.
- Lin, F. R., Yaffe, K., Xia, J., Xue, Q. L., Harris, T. B., Purchase-Helzner, E., Satterfield, S., Ayonayon, H. N., Ferrucci, L., Simonsick, E. M., & Health ABC Study Group (2013). Hearing loss and cognitive decline in older adults. JAMA Internal Medicine, 173(4), 293–299.
- Major, B., & O'Brien, L. (2005). The Social psychology of stigma. Annual Review of Psychology, 56, 393-421.
- Powers, T. A. & Rogin, C. M., (2019). MarkeTrak 10: Hearing aids in an era of disruption and DTC/OTC devices, Hearing Review, 26(8), 12-20
- Privado, J., Carrasco, L. & Duran, R. (2019). Hearing loss: Stigma consciousness, quality of life and social identity, The Spanish Journal of Psychology, 22, E22.
- Shukla, A., Harper, M., Pedersen, E., Goman, A., Suen, J. J., Price, C., Applebaum, J., Hoyer, M., Lin, F. R., & Reed, N. S. (2020). Hearing loss, loneliness, and social isolation: A systematic review. Otolaryngology--Head and Neck Surgery, 162(5), 622–633.
- Wallhagen, M.I. (2009). The stigma of hearing loss. The Gerontologist, 50(1), 66–75.
- Weinstein, B. E., Sirow, L. W., & Moser, S. (2016). Relating hearing aid use to social and emotional loneliness in older adults. American Journal of Audiology, 25(1), 54–61.


