Creative Audiology Problem Solving
Thinking Outside of the Box
In the early days of hearing science, audiologists and hearing scientists would develop solutions to problems by applying scientific knowledge and using a trial-and-error approach. Today, we focus on evidence-based practice, applying knowledge learned in our graduate programs to assist patients with hearing and balance concerns. While having an evidence base for clinical decision-making is vitally important, there are situations that we encounter that may require creative thinking and problem-solving. Here, we present three stories illustrating the benefits of thinking “outside of the box” for our patients.
How much can you fit in an ear?
Bill, a 55-year-old male, presented to our clinic with a classic presbycusis pattern of hearing loss (a mild to moderate high-frequency sensorineural hearing loss) and bilateral tinnitus which was not bothersome. He reported a minor history of occupational noise exposure but no other otologic concerns or relevant audiological history. His primary concern was hearing in the workplace; Bill works as a security guard in a medical facility, primarily working an overnight shift where it is very quiet. As a result, he was concerned about hearing environmental noises on his rounds. After evaluating his communication needs, we decided that a receiver-in-the-canal (RIC) style hearing aid was most appropriate for him.
Bill had one concern with wearing hearing aids – as part of his job, he must use a radio with a unilateral earpiece. The radio was attached to a sound tube that fits over the ear with a ready-wear dome in the ear canal. Here, we had a problem – how do we allow for radio use while continuing to use amplification? To solve this problem, we discussed two options: 1. Setting up a streaming audio system through the hearing aids, with a Bluetooth transmitter attached to his radio, a Bluetooth receiver/streamer on his person, and the hearing aids receiving the streamed audio. 2. Wearing a single hearing aid and using the radio in the contralateral ear. Each of these solutions has drawbacks, though – streaming audio uses a significant battery, and it is unlikely that we could get a full 12-hour shift’s worth of streaming audio from the available hearing aid accessories. Use of a unilateral hearing aid could work, but Bill preferred to wear two hearing aids.
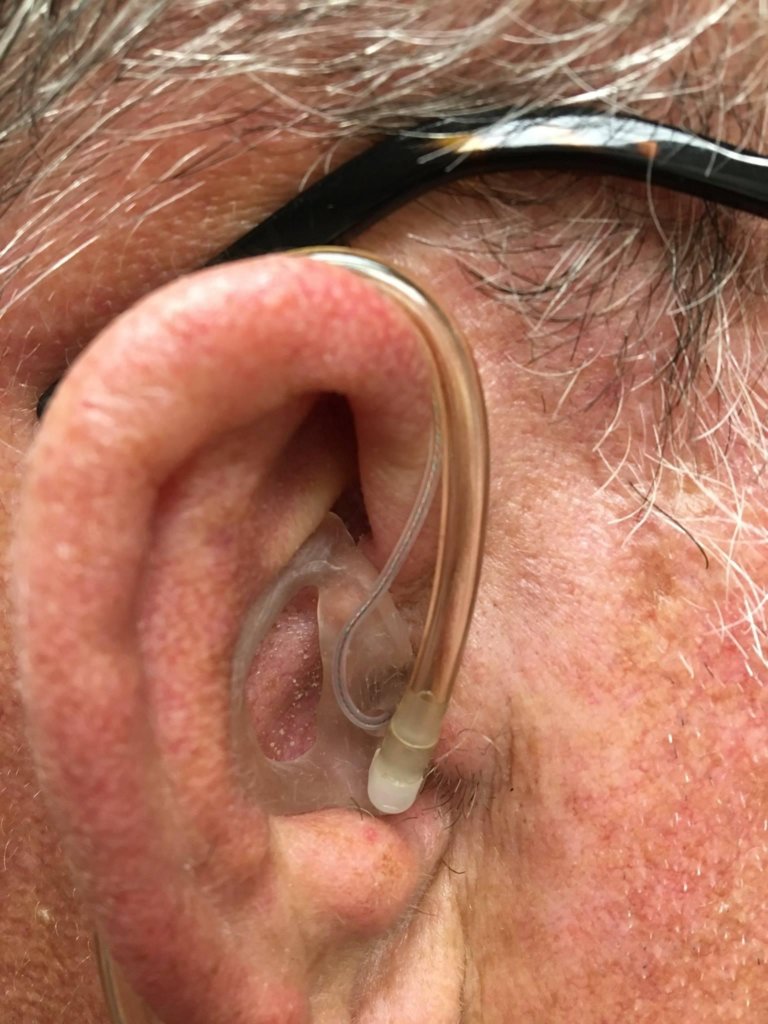
In discussions with Bill, we came to another option; could he wear his hearing aid and his radio simultaneously? The RIC receiver would not fit with the radio earpiece in the ear, but perhaps a custom solution could be made? Fortunately, Bill has a large enough ear canal aperture to try this. We had a custom earmold made, pictured in Figure 1, which can accommodate the RIC receiver, a sound bore for the radio tubing, and a vent. Our custom earmold lab had to work outside their normal parameters, but the earpiece successfully allowed the use of both the hearing aid and the earmold. Bill has now used this device successfully for four years and reported feeling comfortable that he could hear effectively in his job.
Speech-in-noise validation
As a clinic that focuses on performing best practices, we always verify hearing aids using real-ear measures and validate performance using outcomes questionnaires. We also aim to do aided speech-in-noise testing, but sound booth time can be at a premium in our busy clinic. Adding another audiometer with soundfield capabilities was outside our budgets, so we had to find another solution. As audiologists, we usually think only of testing hearing in the sound booth, but there’s no reason that suprathreshold testing needs to be performed in a sound-treated room. Rather, a quiet room with low reverberation could work well for speech-in-noise testing.
To solve this problem of inadequate space for testing, we built a soundfield system in our hearing aid fitting rooms. As shown in Figure 2, this system comprises a single powered studio monitor speaker and a digital music player. A pair of speakers can also be used to split the stimulus and noise for utilizing directional microphones effectively. The digital music player has the speech-in-noise material stored using a lossless compression format (.FLAC or .WAV). We calibrated the system to ensure that at 1 meter, the speech material was being presented at 60 dBA.
In total, this system costs less than $125 ($225 for a two-channel option) and has allowed us to reduce scheduling conflicts in the sound booth. We see no differences between the sound booth and the hearing aid room testing, though we are collecting ongoing data to prove this. We also intend to start using this for all of our suprathreshold cochlear implant testing. Again, a little “out of the box” thinking saved a good bit of time and money and allowed us to remove a barrier for meeting best practices.
Managing autophony in SSCD
Jerry, a 73-year-old male, presented to our clinic with complaints of hearing his own voice too loudly in his left ear, perception of the sound of his eyes moving, and some imbalance. He had a mild hearing loss with a significant air-bone gap in the left ear only. A CT scan of the temporal bones identified left-sided superior semicircular canal dehiscence (SSCD).
In our Otology/Audiology clinic, we see quite a few cases of SSCD, which is characterized by a dehiscence of bone across the superior semicircular canal. SSCD results in a presentation of vertigo, a pseudoconductive hearing loss, and a perception of internal sounds being abnormally loud (autophony). This autophony is due to the dehiscence, which creates a “third window” into the labyrinth, establishing an atypical pathway for bone-conducted sound into the vestibular system and cochlea. As a result, bone-conducted sounds are heard at a lower sound pressure level than in a typical ear. The severity of symptoms varies from severe vertigo and autophony to milder symptoms.
While there are very successful surgical options for repairing this, we also have patients who prefer not to have surgical intervention. Vertigo is sometimes managed by vestibular rehabilitation therapy for these patients, but there is no established intervention for autophony. Jerry elected not to have surgery but remained bothered by his autophony. He was sent to Audiology to evaluate ways to manage this.
On discussion with one of my otology colleagues, we came up with a theory of masking autophony. If abnormally low thresholds cause the autophony for bone-conducted sound, perhaps we could use masking noise delivered through air or bone conduction to increase the patient’s hearing thresholds artificially. Jerry was interested in trying out this theory, so we fit him with both a hearing aid with a multi-channel broadband noise masker and a pair of bone conduction headphones paired to a smartphone playing pink noise. To program the masker in the hearing aid, we asked Jerry to produce the speech sounds that were most bothersome to him and added masking noise at the frequencies which matched the F1 formants for those phonemes. Both the masking in the hearing aid and the broadband masker of the bone conduction headphones effectively reduced Jerry’s perception of his own voice and his eyes moving. Ultimately, Jerry decided that the bone conduction headphones were too conspicuous for daily use and purchased a hearing aid for his left ear with a masker turned on.
This case required us to develop a theory of auditory perception and then find available tools to change the patient’s perception. Because of the success, we are now working on a pilot study of this technique for other patients with SSCD, which we hope to blossom into a formal clinical trial. Exploring existing technology in a new way is a core tenet of effective and efficient medical research practices that audiologists should consider when needed.
As the most knowledgeable and qualified hearing care providers, audiologists are in a unique position to push the boundaries of clinical practice. Don’t be afraid to think creatively - adventurous clinical problem solving can provide patients with the best access to hearing.