Issues in Accessibility – Current Accessibility Strategies in Audiology Practice: A Review of the 2019 CAA Accessibility Survey Results
Accessibility is about creating communities, workplaces, and services that enable everyone to participate fully in society without barriers – this includes audiology clinics. With the adoption of Provincial accessibility legislation (Manitoba, Nova Scotia, Ontario) and the federal Accessible Canada Act, there is now greater support to create accessible environments in Canada. This takes the onus of accessibility from the individual alone to society at large.1Audiologists know that people who are hard of hearing face barriers at work, school, and in their community that hearing aids alone cannot fix. A fundamental service of our profession is to assist people with their hearing needs, and for our clinics to truly reflect this commitment, we must acknowledge that hearing accessibility in community life requires more than basic measurement of hearing in the booth and the fitting of appropriate personal technology. Through our behaviours, policies, outcome measures, and the accessible technologies used in different aspects of our audiology practice, we can demonstrate how accessibility can be improved, and provide information and skills which empower our clients to address their hearing issues in the community. Audiology clinics should serve as a model to the community that the onus of accessibility is not on the individual but is a responsibility of society to reduce barriers to support the full inclusion of people who are hard of hearing. Fundamentally, this sets the stage for the field of audiology’s culture of care and attitude towards people who are hard of hearing.
With or without hearing aids, people who are hard of hearing encounter barriers created by poor acoustics, background noise, poor room lighting, blocked sound and/or line of sight. Multiple assistive technologies and strategies are available to help overcome such barriers, including captioning, hearing loop systems, DM or IR systems, counter loops, speech-to-text apps accessed through WIFI, communication partner skill development, alerting devices, and accessibility policies.
To explore how Canadian audiologists are incorporating accessibility into their clinic facilities and activities, an online survey was sent to CAA members in May 2019, consisting of 16 questions using ‘Survey Monkey.’ This survey asked audiologists to identify the accessible technologies and services audiologists provide at their reception desk area, audiometric testing area, counseling and recommendation methods, outcome measures, website, workplace policies, and behaviours used during public presentations. Audiologists were also asked to provide information on barriers that affect their ability to provide accessible service.
Thirty-three surveys were completed representing audiologists from Alberta, British Columbia, Ontario, Nova Scotia, and Newfoundland & Labrador. Most respondents had 0–5 years of experience (39%) or 21+ years’ experience (39%). For educational background 82% had a master’s degree, 15% had a clinical doctorate (AuD), and 6% had a Doctor of Philosophy (PhD). The primary workplace of respondents was private practice (47%), public or government clinic (12.5%), hospital (31%), and university clinics (9%). Most respondents worked with adults (61%), followed by adults and children (33%), with a smaller representation from audiologists seeing only children (6%). Regarding specialties, the majority of respondents reported providing basic audiometric evaluations (91%) and prescribing and fitting hearing aids (70%) as their primary job roles followed by aural rehabilitation (45.5%), tinnitus (39.4%), electrophysiological testing (33.3%), vestibular assessment (24%), early hearing detection and management (18%), BAHA/middle ear implants (18%), central auditory processing (15%), educational audiology (9%), and industrial audiology (9%). No respondents of the survey reported fitting cochlear implants as part of their job duties.
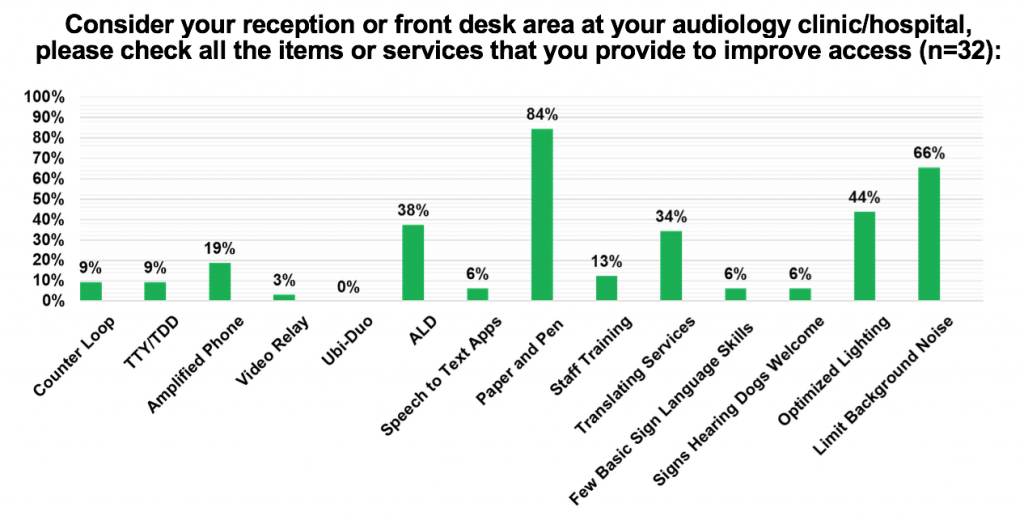
The first question of the survey was related to accessibility at the front desk area of an audiology clinic. An organization’s front desk or reception area is vital to its success because it is the first point of contact for the public. The respondents of the survey reported paper and pen (84%), limiting background noise (66%), and optimizing lighting (44%) as the most common ways to improve accessibility in front desk areas, followed by use of assistive listening devices (38%) and translating services (34%). All other options listed such as counter loops, TTY/TDD, amplified phones, video relay, Ubi-Duo, speech-to-text apps, staff training on communication strategies including basic sign language skills, and signs welcoming hearing dogs all scored below 20% of respondents.
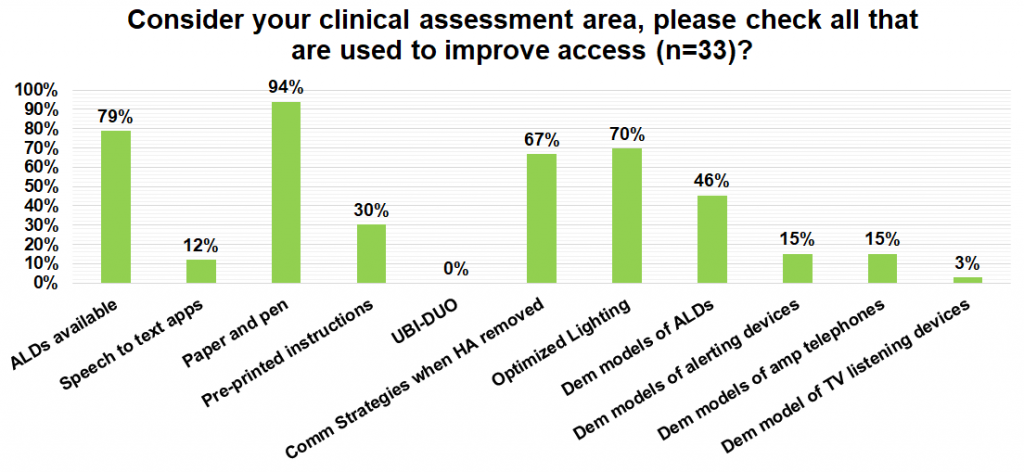
The second question addressed the supports that are available to maximize communication in a clinical assessment area. This is important as this is where the patient’s listening needs are discussed and assessment procedures are explained. Most of the respondents reported using paper and pen (94%) to improve communication during clinical assessment. This was followed by the use of assistive listening devices available in the clinic (79%), optimal room lighting (70%), use of communication strategies when hearing aids were removed (67%), demonstration of assistive listening devices (46%), and use of pre-printed instructions (30%). Additional options listed in the question included the use of speech-to-text apps, UBI-DUO, demonstration models of alerting devices, amplified telephones, and TV listening devices which all scored below 20% of respondents.
The next survey question focused on what accessibility supports audiologists are using during counseling and management recommendations. The supports most commonly discussed were remote microphone or FM systems (88%), funding options (76%), information on communication strategies (76%), ALDs (70%), t-coils (67%), TV listening devices (67%), amplified telephones (64%), writing letters of support (61%), alerting devices (58%), information on support agencies (55%). Less than half of respondents discussed self-advocacy (46%) or speech reading (36%) and less than a quarter reported providing on-site support in the workplace (4%), post-secondary institutions (6%) or in nursing homes (24%).
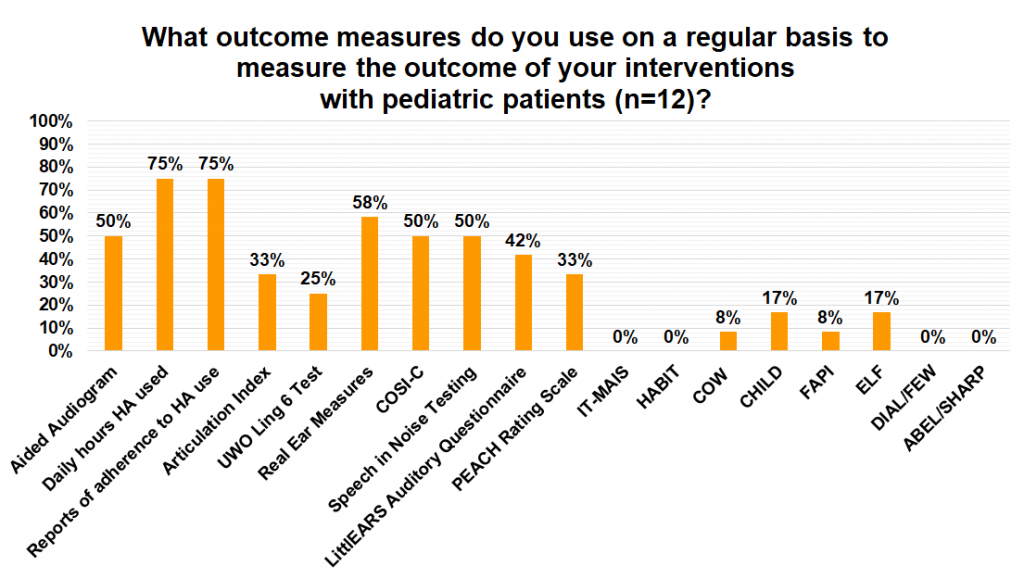
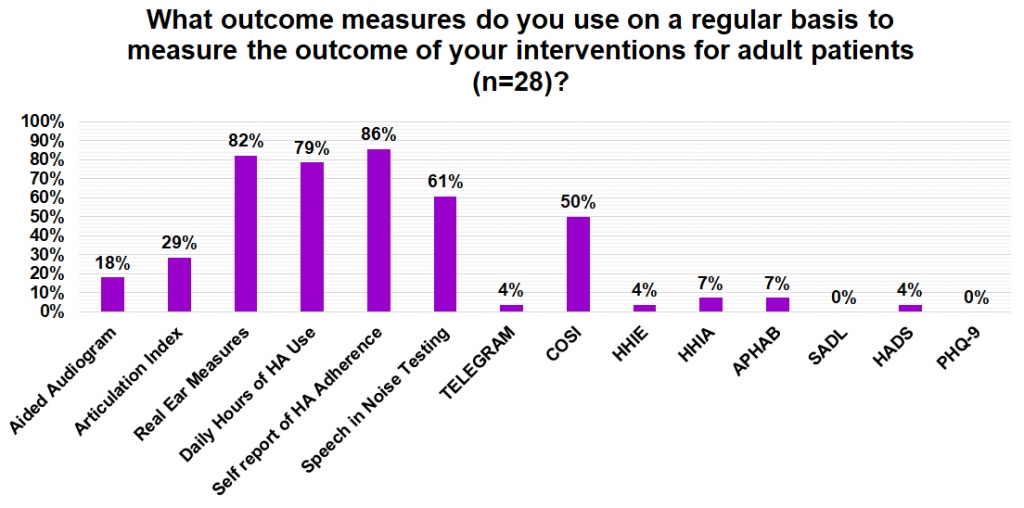
The next two survey questions looked at outcome measures used with pediatric and adult populations. Outcome measures quantify the success of an intervention and the need for further follow-up which is an important aspect of accessibility. For adult patients, the most commonly used measures were self-reports of hearing aid adherence (86%), real-ear measures (82%), self-reports of daily hours of hearing aid use (79%), speech in noise testing (61%), the COSI (50%), the Articulation Index (29%), and aided audiograms (18%). For pediatric patients, the most commonly used measures were parental reports of daily hours of hearing aid use (75%), parental reports of adherence to hearing aid use (75%), real-ear measures (58%), aided audiograms (50%), speech in noise testing (50%), the COSI-C (50%), LittlEars Auditory Questionnaire (42%), the PEACH rating scale (33%), the Articulation Index (33%) and the UWO Ling 6 test (25%).
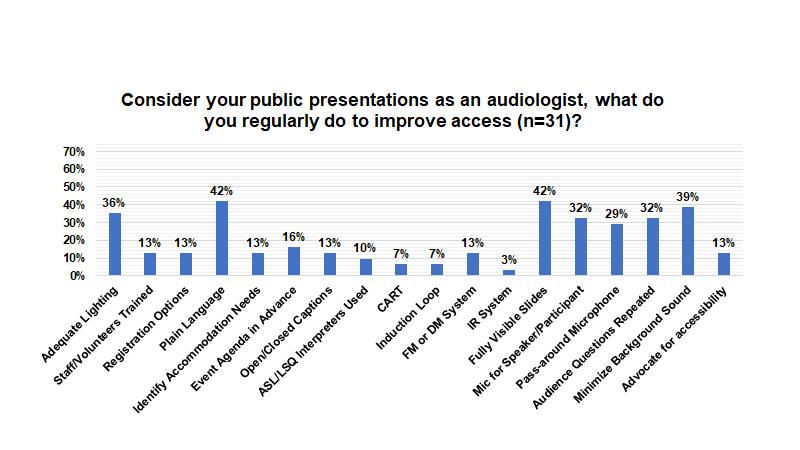
Of all the questions asked about reducing accessibility barriers, public presentations scored the lowest among survey respondents. The two most common measures reported to improve accessibility during presentations were using plain language (42%) and having fully visible slides (42%). Minimizing background noise (39%), having adequate lighting (36%), having a microphone for the presenter or participant (32%), having the presenter repeat audience questions (32%), and using a pass-around microphone (29%) were the next most commonly reported. All other options listed scored less than 20% including using CART (7%), induction loops (7%), FM or DM systems (13%), open/closed captions (13%), having ASL/LSQ interpreters (10%), or identifying accessibility needs ahead of the presentation (13%).
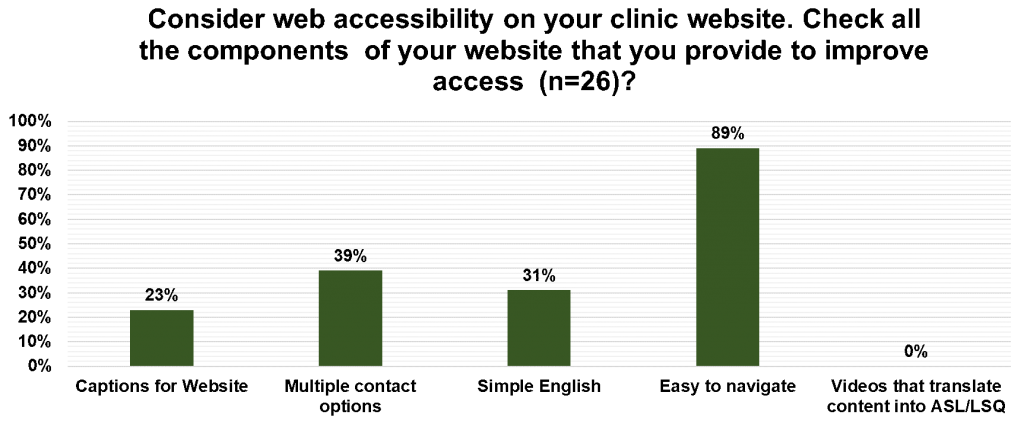
Web accessibility also had low scores in terms of reducing accessibility barriers. Although 26 respondents reported they tried to make their website easy to navigate (88%), a much smaller number offered multiple contact options (such as TTY/DD, video relay services, e-mail, Skype, or text) (38%), content with simple English (30%), closed captions for videos (23%). No respondents reported having videos that translated the written content into ASL/LSQ.
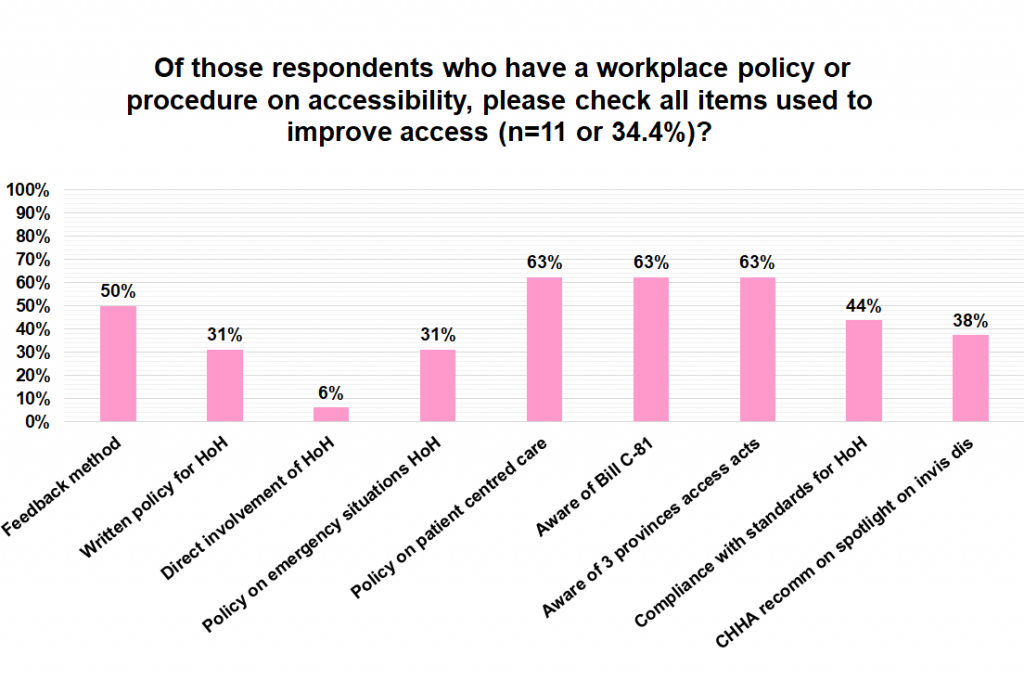
All people are entitled to have workplaces and services in the community that are inclusive and accessible. Workplace accessibility policies and procedures can help raise awareness and define what the issues are to reduce attitudinal, informational and communication, systemic, physical and architectural, and technological barriers for people who are hard of hearing. A small number of respondents reported they had a workplace policy or procedure on accessibility (34%). Of those that did, 63% were aware of Bill C-81 (The Accessible Canada Act) and that three provinces have provincial accessibility acts (Manitoba, Nova Scotia, and Ontario). Regarding feedback, 50% of those that had a policy had a method for the public to provide on-going feedback on how to improve accessibility, 44% made a deliberate effort to be in compliance with accessibility standards, and 38% were aware of the Spotlight on Invisible Disabilities Community Consultation report and the concerns of recommendations outlined from the Canadian Hard of Hearing Association members.
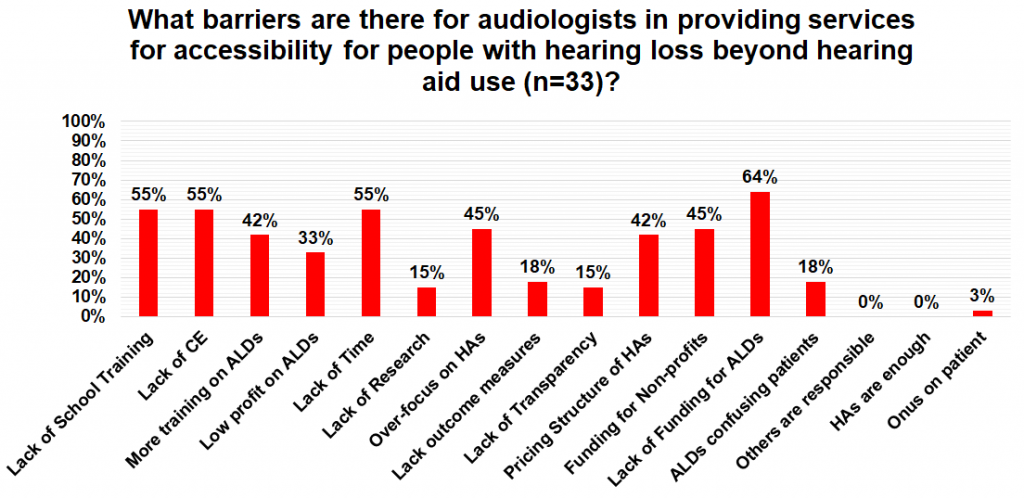
The final question of the survey examined what the barriers were for audiologists to provide accessible audiology services for people with hearing loss beyond hearing aid use. The most common barriers reported were a lack of funding for ALDs (64%), lack of time (55%), lack of CE (55%), lack of school training (55%), lack of financial supports for non-profit groups who provide education about accessibility to the public (45%), an over-focus on hearing aids (45%), more training required on ALDs (42%), and issues with the pricing structure of hearing aids (42%).
Keeping in mind there was a small number of surveys completed (33 respondents), the results indicate a need for improved accessibility services for people who are hard of hearing in audiology clinics. This was based on the fact that a large percentage of possible accessible options surveyed were used by less than half of the respondents. These results also reflect a need and desire from respondents for more educational support on accessibility in university programs and continuing educational opportunities to reduce barriers.
Three main reasons why audiology clinics should choose to make accessibility a top priority for people who are hard of hearing are:
- It is the Right Thing to Do:
- It is the law: Reducing accessibility barriers in the receipt of goods and services, information and communication, public transportation, employment, and education for people with hearing loss is in the process of or is required according to Federal and Provincial accessibility legislation, the National Building Code, the Universal Declaration of Human Rights, and the Canadian Charter of Rights and Freedom.
- It is in our code of ethics: The Canadian Academy of Audiology’s and Speech-Language and Audiology Canada’s code of ethics were both founded on the principles of biomedical ethics of respect for autonomy, beneficence, non-maleficence, and justice. These moral principles should be guiding our behaviours to provide a service that fully addresses the listening needs of people who are hard of hearing.2
- The Consequences for People who are Hard of Hearing:
-
- Public Health Consequences: Hearing loss negatively affects interpersonal communication, psychosocial well-being, and quality of life.3–8 Hearing loss is now the fourth leading cause of years lived with disability9 and the WHO estimates the annual cost of unaddressed hearing loss to be about US$750 billion globally.10 There has been a lot of research examining the connection between hearing loss and downstream conditions such as dementia,11 social and emotional loneliness,12
depression,13 changing family and community engagement,14 and increased risk of falls and other physical disabilities.15
- Public Health Consequences: Hearing loss negatively affects interpersonal communication, psychosocial well-being, and quality of life.3–8 Hearing loss is now the fourth leading cause of years lived with disability9 and the WHO estimates the annual cost of unaddressed hearing loss to be about US$750 billion globally.10 There has been a lot of research examining the connection between hearing loss and downstream conditions such as dementia,11 social and emotional loneliness,12
However, upstream conditions have received less attention. Upstream conditions shift the focus from individual risk factors and behaviours to the societal conditions that can create barriers to healthy living including:
-
-
- The built environment (e.g., poor acoustics, reverberation, background noise, distance, visual obstructions).
- Communication barriers (e.g., inaccessible media, lack of sign language interpreters, lack of note-takers, lack of access to accessible technologies like induction loop systems, FM/DM/IR systems, CART, and alerting systems).
- Policy barriers (e.g., lack of awareness or enforcement of existing laws and regulations that require programs and activities to be accessible to people who are hard of hearing such as denying reasonable accommodation to workers who are hard of hearing or denying access to programs or services as a result of physical barriers in the built environment).
- Programmatic barriers (e.g., limiting the effective delivery of a public health or healthcare program such as an audiology clinic for people who are hard of hearing).
- Social barriers including the conditions where people are born, grow, work, live and age (e.g., providing support for an employer or employee, nursing home resident, or student at a post-secondary institution who is hard of hearing).16
-
If upstream conditions for people with hearing loss are not addressed, it may enable the onset of the downstream conditions mentioned above.
- Participation and Activity Limitations: Another factor to consider in determining the importance of reducing accessibility barriers is to examine current trends in the workplace and post-secondary institutions in Canada for people who are hard of hearing. The Statistics Canada Participation and Activity Limitation Survey (2006) found:
- Workplace: 33.2% of employed respondents reported that hearing loss limited the amount or kind of work they could perform and 32.3 % stated that it made it difficult to advance or change jobs. Of the 23.4% not participating in the labour force, 62.5% reported they were completely prevented from working, while 29.0% stated it affected their ability to look for work. Of those respondents who were retired, 39.7% reported their retirement had not been voluntary and 51.3% were completely prevented from working as a result of their hearing loss. These results indicate that more support is needed for people who are Deaf/deaf and hard of hearing in the workplace.
- Post-secondary institutions: Adults aged 15 to 64 with a hearing disability were more likely than those without any type of disability to have not completed high school (23.0% versus 13.1%) or to have a postsecondary qualification (50.3% versus 61.1%). Of the 9.4% of participants who reported that they were currently or had recently been in school, 84.2% stated that their educational experiences were directly impacted by their disability. These impacts included: needing to change their choice of courses, taking fewer courses, and feeling excluded due to their disability. Of the 24.6% survey participants who required some sort of education aid or service, 58.8% reported that all of their needs had been met, 38.6% reported that at least some of their needs had been met, while 2.6% reported that none of their needs had been met.17 These results indicate that more support is needed for people who are Deaf/deaf and hard of hearing in post-secondary institutions.
The statistics discussed above demonstrate the need for society to re-evaluate the services that are provided for people who are hard of hearing, to continue to collect data on these outcomes, and to monitor barriers to continually improve future outcomes.
- The only point of contact: Audiology clinics are typically the first point of contact for individuals seeking out hearing healthcare. We need to educate people about all of their hearing health care options and fully address their listening needs as they may not get this important information or service anywhere else.
- Communication Breakdowns in a Clinical Setting: Research shows that hearing loss can hurt clinical communication in hospital and clinical settings. Failures in clinical communication are considered to be the leading cause of medical errors. A study by Cudmore et. al., reported general mishearing, consultation content, communication breakdown, the setting itself, and the use of language as common themes in miscommunication in a clinical setting. Hearing aids are not always enough depending on factors such as speech comprehension, background noise, and room acoustics, therefore we need to ensure we are addressing these barriers to reduce the need for increased attention, concentration, and listening effort.18In 2016, Weinstein reported, ‘we must focus on helping to improve our patients’ ability to cope with environmental demands and provide solutions our patients must adopt to self-manage in these situations. Because the intersection is a dynamic one, we must constantly re-evaluate our patients’ residual disability, functional status, self-efficacy, and adherence.’19
-
- The Business and Community Benefits:
- Economic Benefits: Not only is providing an accessible service the right thing to do, it is also the smart thing to do from a business model perspective because it meets legal requirements, improves quality of service, improves retention and loyalty, demonstrates corporate social responsibility, creates an advantage over competitors, and improves the bottom line. The Conference Board of Canada reports20:
The number of Canadians living with a physical disability that impairs their mobility, vision, or hearing will rise from 2.9 million to 3.6 million over the next 13 years, nearly double the pace of the population as a whole. Real spending by this group will rise from 14 to 21% of the total consumer market and improvements to workplace access would allow 550,000 Canadians with disabilities to work more, increasing GDP by $16.8 billion by 2030. - Adopting a Lifespan Approach: In age-friendly communities, the policies, services, and structures related to the physical and social environment are designed to help seniors ‘age actively' in a workplace or in the community. The environment should be set up to help seniors live safely and stay involved.21 To identify and manage hearing loss, Weinstein recommends that audiologists need to revisit our scope of practice and redirect our professional activities with the adoption of a lifespan approach.22 Audiologists can support age-friendly workplaces and communities by understanding universal design principles and applying them in our clinical work. The foundation of these principles can be found through the work of Fok, Shaw, Jennings and Cheesman who adapted universal design principles for people with hearing loss.23,24Pichora-Fuller et al. reported the importance of adopting a healthy aging perspective that focuses on facilitating active social participation by older adults. These initiatives could “increase awareness of the importance of hearing health, better integrate hearing health care into the larger health care picture, increase uptake of amplification devices and other forms of audiologic rehabilitation, and mandate public policies and environmental accommodations (e.g., ambient noise controls and access to written information in public spaces).”25 What better way to promote an age-friendly community and facilitate active social participation by older adults than to be a model in our audiology clinics for other businesses and services in the community?
- Economic Benefits: Not only is providing an accessible service the right thing to do, it is also the smart thing to do from a business model perspective because it meets legal requirements, improves quality of service, improves retention and loyalty, demonstrates corporate social responsibility, creates an advantage over competitors, and improves the bottom line. The Conference Board of Canada reports20:
Overall, these survey results demonstrate the need for a paradigm shift within the field of audiology towards a more accessible service with an emphasis on greater educational and funding supports for Audiologists to create this improvement.
References
- Employment and Social Development Canada. Making and Accessible Canada for People with Disabilities; 2018. Retrieved from: https://www.canada.ca/en/employment-social-development/programs/accessible-people-disabilities.html
- Beauchamp TL and Childress JF. Principles of Biomedical Ethics (5th ed.). New York City, NY: Oxford University Press; 2001.
- Mason A and Mason M. Psychologic impact of deafness on the child and adolescent. Prim Care 2007;34:407–26. doi: 10.1016/j.pop.2007.04.003.
- Shield B. Evaluation of the social and economic costs of hearing impairment: a report for Hear-it London: London South Bank University; 2006. Retrieved from https://www.hear-it.org/sites/default/files/multimedia/documents/Hear_It_Report_October_2006.pdf
- Kotby MN, Tawfik S, Azizm and Taha H. Public health impact of hearing impairment and disability. Folia Phoniatr Logop 2008; 60:58–63. doi: 10.1159/000114646.
- Karchmer MA and Allen TE. The functional assessment of deaf and hard of hearing students. Am Ann Deaf 1999;144:68–77. doi: 10.1353/aad.2012.0468.
- Venail F, Vieu A, Artieres F, et al. Educational and employment achievements in prelingually deaf children who receive cochlear implants. Arch Otolaryngol Head Neck Surg 2010;136:366–72. doi: 10.1001/archoto.2010.31.
- Schroeder L, Petrou S, Kennedy C, et al. The economic costs of congenital bilateral permanent childhood hearing impairment. Pediatrics 2006; 117:1101–12. doi:10.1542/peds.2005-1335.
- Livingstone G, et. al. The Lancet Commissions 2017;390(10113) P2673–2734. Retrieved from: https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(17)31363-6/fulltext
- World Health Organization. Global costs of unaddressed hearing loss and cost-effectiveness of interventions: a WHO report. Geneva; 2017. Licence: CC BY-NC-SA 3.0 IGO. Retrieved from: http://apps.who.int/iris/bitstream/handle/10665/254659/9789241512046-eng.pdf
- Thomson RS, Auduong P, Miller AT, and Gurgel RK. Hearing loss as a risk factor for dementia: A systematic review. Laryng Investigat Otolaryngol 2017;2(2):69–79. http://doi.org/10.1002/lio2.65.
- Weinstein B, Sirow LW, and Moser S. Relating hearing aid use to social and emotional loneliness in older adults. Am J Audiol March 2016(5)54–61. doi:10.1044/2015_AJA-15-0055
- Li C-M, Zhang X, Hoffman HJ, et al. Hearing impairment associated with depression in US adults, National Health and Nutrition Examination Survey 2005–2010. JAMA Otolaryngol Head Neck Surg 2014;140(4):293–302. Retrieved from: http://doi.org/10.1001/jamaoto.2014.42
- Pichora-Fuller MK, Mick P, and Reed M. Hearing, cognition, and healthy aging: social and public health implications of the links between age-related declines in hearing and cognition. Semin Hear 2015;36(3):122–39. Retrieved from: http://doi.org/10.1055/s-0035-1555116
- Lin FR and Ferrucci L. Hearing loss and falls among older adults in the United States. Arch Intern Med 2012;172(4):369–71. Retrieved from: http://doi.org/10.1001/archinternmed.2011.728
- Centers for Disease Control and Prevention. Common Barriers to Participation Experienced by People with Disabilities. 2019. Retrieved from: https://www.cdc.gov/ncbddd/disabilityandhealth/disability-barriers.html
- Statistics Canada. The 2006 Participation and Activity Limitation Survey: Disability in Canada. Statistics Canada Catalogue no. 12-89-628-X. Ottawa. Version updated Feb 2009. Ottawa; 2010. Retrieved from: https://www150.statcan.gc.ca/n1/pub/89-628-x/2009012/fs-fi/fs-fi-eng.htm
- Cudmore V, Henn P, O’Tuathaigh CMP, and Smith S. Age-related hearing loss and communication breakdown in the clinical setting. JAMA Otolaryngol Head Neck Surg 2017; doi:10.1001/jamaoto.2017.1248
- Weinstein, B. Management of psychosocial challenges posed by communication breakdowns. Hear J 2016; 69(3)8–10. doi: 10.1097/01.HJ.0000481807.28828.ec
- Gibbard R, Desormeaux M, Persaud P, and Wright R. The Business Case to Build Physically Accessible Environments. Conference Board of Canada; 2018. Retrieved from: https://www.conferenceboard.ca/temp/ab4e1174-7848-454e-aa54-7c3ec2c3c8a4/9434_Accessible-Environs_RPT_Accessible.pdf
- Government of Canada. Age-Friendly Communities; 2016. Retrieved from: https://www.canada.ca/en/public-health/services/health-promotion/aging-seniors/friendly-communities.html
- Weinstein B. A life course approach to hearing care – part 1. Hear J 2018;71(1). doi: 10.1097/01.HJ.0000529844.93623
- Fok D, Shaw L, Jennings MB, and Cheesman M. Universal accessibility and usability for hearing: Considerations for design. Can Acoust 2007;35:3.
- Jennings MB. Hearing Accessibility and Assistive Technology Use by Older Adults: Application of Universal Design Principles to Hearing. In Louise Hickson ed. Hearing Care for Adults 2009- The Challenge of Aging. (pp. 249-254). Proceedings of the Second International Adult Conference. Second International Adult Conference, Chicago, United States, 16-18 November 2009. Staefa, Switzerland: Phonak.
- Pichora-Fuller MK, Mick P, and Reed M. Hearing, cognition, and healthy aging: social and public health implications of the links between age-related declines in hearing and cognition. Semin Hear 2015;36(3):122–39. Retrieved from: http://doi.org/10.1055/s-0035-1555116


