Minimizing the Risk of Infection in the Hearing Healthcare Environment
Hearing is Essential
Communication has become even more critical as social distancing, reliance on phone calls and videoconferencing have become the norm and staying connected is more challenging. As practices re-open or expand services to return to “normal”, how can we prepare to provide exceptional in-person care in a safe, responsible way? It begins with establishing or updating an infection control protocol to ensure a safe environment for the provision of hearing healthcare services.
What is Infection Control?
It is the development, implementation and consistent execution of procedures designed to manage the clinical environment and reduce the potential spread of disease1. It assumes every microbe is potentially infectious and requires controlling transmission between people and between people and the work environment. COVID-19 has demonstrated the impact that an infectious disease can have and the need to guard against such infections in a healthcare environment.
Infection Control is critical in hearing healthcare because of the patient populations we serve, the equipment we use and the services we provide. The comorbidities of hearing loss; diabetes, hypertension, respiratory and heart disease have also proven to be especially vulnerable conditions for persons with COVID-19. Daily, we contact numerous surfaces, share equipment with others and have close physical contact with our patients as we serve their needs. How should we control our behaviors and work environment to ensure the health and safety of both patients and staff?
How is Disease Transmitted?
The transfer of disease typically involves the eyes, ears, nose, and mouth. There are four modes for the transmission of disease: Contact, Vehicle, Airborne and Vector borne. Contact transmission is the most common mode and has three subcategories: Direct, Indirect and Droplet Contact. Droplet Contact, involves transmission through particles expelled via coughing, sneezing or talking and is the main mode of transmission for COVID-19. The distance these particles can travel has led to social/physical distancing and facemask recommendations in many communities.
How Do We Protect Ourselves and Others?

Practices offering patient care should have a written infection control plan in place. It should be evaluated to determine if updates need to be made to reflect the evolving guidelines related to COVD-19. It is critical for all staff to recognize that precautionary measures are required and that work practice protocols involving use of PPE, sanitizing and safe behaviors be established for all office procedures. Practicing hand hygiene; washing hands often with soap and water for at least 20 seconds remains the first line of defense against the spread of disease. Hand sanitizer containing 60–95% alcohol is an acceptable alternative when soap and water are not an option.
The use of PPE (Personal Protective Equipment) such as gowns, glasses, gloves and masks has expanded during the pandemic. Gowns and protective glasses should be prioritized any time care activities provide opportunity for infectious microbes to transfer to skin or surfaces. Gloves should be worn when in contact with patients, or their products such as hearing aids or accessories and while cleaning/disinfecting surfaces. It is important to consider nitrile or non-latex gloves to avoid latex allergies and potential chemical interaction with impression materials that could prevent the impression from setting up.
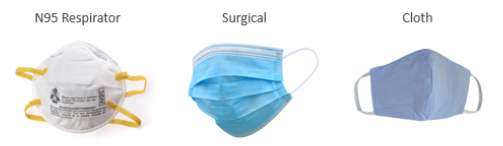
The use of face masks is recommended whenever a 2-meter distance cannot be maintained to protect others from the droplet particles that may carry infection. N95 masks, when fit properly, are designed to filter 95% of the smallest particles in the air and should be reserved for procedures requiring close patient contact or for front line workers at highest risk of exposure. Surgical masks, often blue and white, are fluid resistant, can protect from larger respiratory droplets and are appropriate for general use, especially when social distancing. Cloth masks are an acceptable option when social distancing is difficult to maintain. As shortages of PPE have persisted, the use of cloth masks, even of the homemade variety and alternative gown and protective glasses may be considered.
An unfortunate discovery with facemask use has been the negative impact on speech understanding and the implications for the hearing impaired. A recent study compared listening comprehension while masked with N95, surgical and cloth face masks. It determined masks act as a low pass filter, attenuating 2000-7000 Hz and from 3-4 dB for the common surgical mask to 12 dB for the N95.2 Clear mask options have become commercially available and should be considered to help minimize the communication gap when wearing masks. Clear face shields are an acceptable alternative when masks are unavailable and offer the advantage of a larger visual field and the ability to provide visual cues. The face shield should cover down to the chin and below.3
Now is also the time to evaluate professional attire and minimize risk of clothing contamination. Consider short sleeves, eliminating lab coats, neckwear and jewelry such as watches, rings and bracelets for the time being to minimize contamination and aid in good hand hygiene. Consider removing work clothing and shoes prior to entering the home and washing them separately from other laundry.
Managing the Work Environment
Surfaces in all office areas that come in direct or indirect contact with hands or may be splashed with bodily substances or fluids, must be cleaned AND disinfected on a regular basis. Equipment and tools that contact potentially infectious agents must be sterilized.

What’s the difference between cleaning, disinfection and sterilization? Each term has a very specific definition and requires the use of the correct solution to meet the legal requirements for use defined by the appropriate regulatory agency.
Cleaning involves removing the gross contamination from an object or surface without killing germs. Cleaning may be accomplished with soap and water, tissue or brush and is the precursor to disinfection.
Disinfection kills a specific number of germs, as specified by the level of disinfectant used and is required for “non-critical” items and surfaces; those that do not contact blood or potentially infectious substances. Healthcare practices should use a hospital-grade disinfectant that could be a towelette, spray or soaking solution. Although rubbing alcohol is considered a disinfectant, it is not recommended due to its chemical composition and potential to denature materials and devices used in the hearing healthcare environment. A list of approved disinfectants for use against SARS-2 (COVID-19) 4 can be found here https://www.canada.ca/en/health-canada/services/drugs-health-products/disinfectants/covid-19/list.html#tbl1.
Sterilization kills 100 percent of the germs, 100 percent of the time and is required for “critical” instruments that could break the skin (curettes, wax loops) or be contaminated with potentially infectious materials such as blood, mucous or other bodily substances. Cold sterilization, most often used in hearing healthcare, is accomplished by soaking instruments in a solution that is 2% glutaraldehyde or in 7.5% hydrogen peroxide, the only approved solutions for sterilization. 5 Gloves MUST be worn, and glasses considered when using glutaraldehyde and sterilized instruments should be rinsed prior to direct contact with skin. CaviCide is a popular, easy to use/reuse sterilization solution. Sporox, a 7.5% hydrogen peroxide solution, can be reused, making it an ideal sterilant for the hearing healthcare environment.
Prepare the Clinical Environment and Patient Experience

For every task, what is needed to make the entire service experience safe? What is needed to communicate and follow the necessary safety procedures? It starts with a written infection control plan that includes all necessary safety measures and reflects evolving changes as a result of COVID-19. Staff must be trained on appropriate procedures for PPE use, hand hygiene, distancing and sanitizing procedures.6 Outline procedures for in-person visits (including curbside and drop off services) and communicate expectations for patients including PPE, calling prior to entry, limitations to companions and hand hygiene guidelines while on the premises. Place signage that communicates these expectations throughout the practice.
Evaluate the practice from the front entry to the waiting area, hallways, treatment, and lab areas, to minimize risk. Limit entry/exit points, reduce contact surfaces such as furniture, minimize community objects (i.e. magazines, brochures, pens) and adjust seating and traffic areas to encourage social distancing of 2 meters. Air flow, especially in test booths should be evaluated; air filters changed regularly and high efficiency HEPA filters considered to remove most air particles. Leave doors open when possible to improve air flow and limit touch points.
How Can We Re-Think Our Patient Interaction?
- Modify your stance to position yourself at ear level or slightly behind the patient to distance from the patient’s mouth
- Consider remote or room-to-room programming, taking advantage of the distance provided by wireless programmers
- Refrain from sharing equipment, keyboards, phones and tools with co-workers
Establishing Trust
The public is more aware of infection control and hand hygiene than ever before. Your patients will be watching to see the steps you and your practice are taking to keep them safe.
- Communicate all the safety protocols your office has in place
- Complete hand hygiene procedures before/after the session in front of the patient and encourage them to do the same
- Consider offering PPE for your patients
- Clean and disinfect products and instruments in front of the patient
There is no playbook for the profound change our world has experienced as a result of COVID-19. By practicing infection control protocols and developing a safety plan for ourselves and our workplace, we can communicate to our patients that we have their health and wellbeing in mind.
References
- Bankaitis AU, Kemp R. Infection Control in the Audiology Clinic. Oaktree Products; 2005
- Goldin A, Weinstein B, Shiman N, How do medical masks degrade speech recognition: Hearing Review 2020.27.05
- Perencevich E, Diekema D, Edmond M., Moving personal protective equipment into the community. JAMA 2020. Published online 4/29/20
- Health Canada. Hard-Surface Disinfectants And Hand Sanitizers (COVID-19): List Of Disinfectants With Evidence For Use Against COVID-19 Available at: https://www.canada.ca/en/health-canada/services/drugs-health-products/disinfectants/covid-19/list.html#tbl1
- : American Academy of Audiology: Infection Control Task Force. Infection Control in Audiological Practice. Available at: https://www.audiology.org/publications/guidelines-and-standards/infection-control-audiological-practice
- Public Health Canada. Infection Prevention and Control For COVID-19: Interim Guidance for Outpatient and Ambulatory Care Settings. Available at: https://www.canada.ca/en/public-health/services/diseases/2019-novel-coronavirus-infection/guidance-documents/interim-guidance-outpatient-ambulatory-care-settings.html#_Toc40651320

